Home » Services » Interventional procedures » Pelvic congestion syndrome
Pelvic congestion syndrome
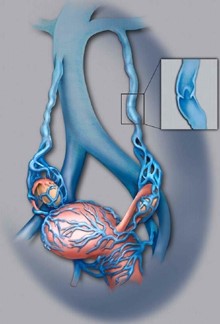
Pelvic congestive syndrome (PCS) is one of the causes of chronic pelvic pain, a condition very common in women that can potentially lead to significant disability. Approximately one third of all women will suffer from chronic pelvic pain at some point in their lives. Chronic pain, by definition, lasts longer than six months and is not related to a woman’s menstrual cycle.
There are many different causes of chronic pelvic pain and this can make the diagnosis more difficult. Pelvic congestive syndrome (PCS) must be considered if the pain worsens while sitting or standing and is relieved by lying down. Some patients may also experience pain during urination (dysuria) or during / after sexual activity (dyspareunia).
PCS is associated with what is known as dilatation of the ovaries and pelvic veins. This can result in varicose veins in the pelvis, thighs, buttocks or vaginal area. Pelvic cohesive anchor is a complex medical condition and requires a multidisciplinary team approach to treatment and assessment.
Symptoms of pelvic congestive syndrome
Symptoms of PCS can include any of the following:
- Dull, aching or “pulling” pain in the pelvis or lower back, especially in a standing position and worse during menstruation
- Irritable bladder that sometimes leads to stress incontinence
- Irritable bowel syndrome (recurrent abdominal pain and diarrhea alternating with periods of constipation)
- Deep dyspareunia (discomfort during or after sexual intercourse)
- Vaginal or vulvar varicose veins (bulging veins around the anus)
- Varicose veins at the top of the inner thigh or the back of the thigh
Causes of pelvic congestive syndrome
The cause of pelvic congestive syndrome is unclear. However, the possibility of anatomical or hormonal abnormalities or dysfunction may contribute to the development of this syndrome. Most of the women affected are between the ages of 20 and 45 and have multiple previous pregnancies.
One theory is that hormonal changes and weight gain along with anatomical changes in the pelvic structure during pregnancy can cause an increase in pressure in the ovarian veins. This can weaken the vein wall leading to dilatation. Estrogen can also weaken vein walls, predisposing women to pelvic congestive syndrome.
What we do know is that in normal veins, blood flows from the pelvis to the heart into the ovarian vein, and the valves inside the vein prevent it from flowing backwards. When the ovarian vein dilates, the valves do not close properly. This results in backflow of blood, also known as “reflux”. When this happens, blood aggregates within the pelvis. This in turn leads to pelvic varicose veins and clinical symptoms of heaviness and pain.
Risk factors
Most women with pelvic congestion syndrome are under the age of 45 and are in reproductive age. Certain factors can put a woman at higher risk for this condition, including:
- Multiple (2 or more) pregnancies
- Presence of a uterus with a “tip” (retroverted)
- Fullness of veins in the legs
- Polycystic ovaries
- Increased hormones or dysfunction
Diagnosis
Several diagnostic tests may be useful to assess pelvic congestive syndrome.
Ultrasound: Ultrasound of the abdomen and pelvis can help assess PCS. With the help of ultrasound, we can directly visualize reflux in the ovarian veins and identify dilated pelvic veins.
Computed tomography (CT) or magnetic resonance imaging (MRI): In some situations, ultrasound alone may not provide all the necessary information and your doctor may want to obtain additional images. CT and MRI are used to visualize abnormal veins in the pelvis, look for other abnormalities, and assess surrounding structures.
Pelvic venography: The most basic imaging method for diagnosing PCS, this minimally invasive procedure is performed in a hospital by a vascular specialist. A catheter (tube) enters the venous system from the groin or neck, and an X-ray is then used to guide the catheter into the ovarian vein. Iodine-based dye is injected into a vein and images are obtained. Pelvic venography can also be used as a treatment in combination with a non-surgical, minimally invasive procedure known as pelvic embolization. At the decision of your surgeon, these procedures can be performed together or at different times.
Treatment options
Ovarian vein embolization
Ovarian vein embolization is a minimally invasive treatment for pelvic congestion syndrome, a painful condition that results from the presence of enlarged or dilated pelvic veins. It helps relieve pain by using a recording guide and a catheter to close the defective veins so that they can no longer increase with blood. Embolization is a highly effective way to control bleeding and is much less invasive than open surgery.
Pelvic congestion syndrome, also known as ovarian vein reflux, is a painful condition that results from the presence of varicose veins in the pelvis. The condition is caused by valves in the veins that help return blood to the heart against gravity that becomes weakened and does not close properly, allowing blood to flow back and unite in the vein causing pressure and bulging veins.
During this procedure, the interventional radiologist inserts a catheter into the femoral vein and abnormal ovarian and pelvic veins. Catheterization requires only a small incision in the skin for insertion and an X-ray-guided catheter to the target area. The catheter delivers coils that carry blood-clotting agents and seal the damaged vein. Sclerosing agents are injected into the varicose veins of the pelvis, and small metal coils or plugs are placed to prevent the flow into the ovarian vein. This prevents reversal of flow in the abnormal vein, which reduces the pressure in the dilated pelvic veins.
The use of a recently developed agent allows the radiologist to block even the smallest veins that were previously inaccessible.
When to return to normal activities after ovarian vein embolization
This procedure is usually performed on an outpatient basis, and patients can return to normal activity in a few days. After ovarian vein embolization, approximately 75 percent of patients will experience an improvement in symptoms.
Before ovarian vein embolization intervention
Tell your doctor if there is a possibility that you are pregnant and discuss recent illnesses, health conditions, allergies, and medications you are taking, including herbal supplements and aspirin. You may be advised to stop taking aspirin, vitamin E, non-steroidal anti-inflammatory drugs or blood thinners a few days before the procedure. You should not eat or drink after midnight if you have an intervention the next day. Plan to be admitted to the hospital in the morning, leave your jewelry at home and wear loose, comfortable clothes. You may be required to wear a hospital gown.
