Home » Arrhythmia Center
Arrhythmia Center
The Arrhythmia Center of Pulse Cardiology Center is dedicated to providing a complete spectrum of care to patients with heart rhythm disorders in Serbia and the region. Our cardiac electrophysiology specialists at the Arrhythmia Center are trained experts who are dedicated to diagnosing heart rhythm disorders and providing comprehensive evaluation and treatment to patients with arrhythmias, atrial fibrillation (AFIB), and other complications associated with heart rhythm disorders.
The Arrhythmia Center offers patients with heart rhythm disorders the opportunity to undergo all necessary testing, examinations, interventions, and additional care in one place.
At the Pulse Cardiology Center within the Arrhythmia Center, we offer the following services:
- Consultation with an arrhythmologist
- Medication therapy
- Inpatient care
- Pacemaker monitoring
- Pacemaker battery replacement
- All diagnostic methods (ECG, Holter monitoring, Loop recorder)
- Interventions: Pacemaker and ICD defibrillator implantation, cardioversion.
TEAM OF THE ARRHYTHMIA CENTER
Our team is composed of experts who have decades of combined training, education, and work experience. All our specialists (cardiologist, interventional cardiologist, cardio-electrophysiologist) provide state-of-the-art treatment for arrhythmia conditions using a comprehensive approach that is unparalleled in this field. Pulse, with its team, provides the most advanced treatments for complex arrhythmias and other complications of arrhythmias, using advanced medical therapies, 3-D computerized mapping techniques (ablation procedures), implantation of all rhythm devices such as pacemakers and defibrillators, supported by advanced imaging technology and the use of state-of-the-art equipment. The Pulse Cardiology Center’s Cath-lab (angiography room) is the most modern operating room of its kind in the country.
The Head of the Arrhythmia Center is our renowned expert Prof dr Siniša Pavlović, the rest team members are Head of the Electrophysiology Department at Military Medical Academy – MD Ivica Đurić, MD Aleksandar Cicović – Interventional Cardiologist, MD. Vanja Koić – Interventional Cardiologist.
What is cardiac electrophysiology?
Cardiac electrophysiology (EP) is a specialty that focuses on the timing of the heart’s electrical system, as well as the diagnosis and treatment of irregular heartbeats or arrhythmias, also known as atrial fibrillation (AFIB).
The expertly trained, certified cardiologists at the Center for Arrhythmia have completed an additional one – to two year training program in clinical cardiac electrophysiology in addition to their cardiology subspecialization.
When to visit an electrophysiologist?
Patients with simple palpitations to complex arrhythmias are referred by their primary care physician or cardiologist to the Center for Arrhythmia for consultations regarding their heart rhythm condition. These may be newly diagnosed patients with atrial fibrillation (AFIB) or patients who may require additional treatment options to manage their arrhythmia.
Patients can schedule an appointment with one of our doctors.
WHAT CAUSES ARRHYTHMIAS
Heart rate or rhythm is very important for the health of our heart. It is extremely important that it is appropriate so that the heart can perform its pumping function. Neither faster nor slower heart rate are usually good for the heart and the patient in general, although they can sometimes be physiological, or harmless. This will of course depend on many factors and only a cardiologist can tell you after a detailed analysis whether your heart needs treatment.
Arrhythmia is a condition where there is a disturbance in the speed or rhythm of the heart’s contractions. During arrhythmia, the heart can beat too fast, too slow, or with an irregular rhythm. Accelerated heart rate is called tachycardia, and slowed heart rate is called bradycardia.
Most arrhythmias are harmless, but some can be serious or even fatal. When the heart beats too fast or too slow, or with an irregular rhythm, its pumping function is reduced, and it cannot pump enough blood to all parts of the body. This can damage the brain, heart, and other organs.
To understand heart arrhythmias, it is necessary to familiarize oneself with the conduction system of the heart.
Electric impulses in the heart lead to contractions of the cardiac muscle (myocardium). Impulses are generated in the right atrium in the so-called SA node, which is also called the “natural pacemaker of the heart.” The impulse is then transmitted to the AV node located in the lower part of the right atrium, where impulses are slowed down before entering the ventricles, and then through the so-called bundle of HIS to the Purkinje fibers. Slowing down of impulses in the AV node is significant because it allows the atria and ventricles to contract at different times. This network conducts impulses to the muscle of the ventricles and causes their contraction (contraction). This contraction allows the heart to pump blood into the lungs and other parts of the body. If there is a failure to create impulses in the SA node, impulses will be generated in the AV node or lower structures but at a slower rate.
The SA node sends impulses at a specific rate (heart rate). The normal heart rate at rest is 60-100 beats per minute. However, the heart rate changes during physical activity, sleep, stress, or hormonal factors. During sleep, the heart rate can drop to 40 beats per minute, and during physical activity, it can increase to 160 beats per minute.
What can cause arrhythmias?
CAUSES BY THE HEART
CAUSES BY OTHER ORGANS – diseases of the thyroid and adrenal glands, lung, kidney, digestive system, nervous system…
GENERAL DISORDERS IN THE BODY (loss of minerals and fluids, taking certain medications (Digitalis, diuretics, antiarrhythmic drugs, etc.), consumption of drugs, alcohol, smoking, elevated body temperature, decreased blood pressure, decreased oxygen concentration in the blood, etc.).
RISK FACTORS FOR ARRHYTHMIAS
- High blood pressure
- Diabetes
- Coronary artery disease
- Sleep apnea
- Congestive heart failure
- Peripheral vascular disease
- Following cardiac surgery
- Weakened heart muscle – low ejection fraction
- Heart valve disease – even if surgically corrected
- Excessive alcohol or caffeine consumption
SYMPTOMS OF ARRHYTHMIAS
Symptoms can vary from patient to patient, but it can feel like sudden fluttering of the heart, heartbeats become irregular and faster than normal.
- Shortness of breath – especially during physical activity
- Feeling of weakness during exercise
- Chest pain
- Palpitations
- Dizziness
- Fainting
- Fatigue
- Anxiety
CAUSES OF ARRHYTHMIAS
The cause may not be obvious or may be associated with other health conditions such as:
- Coronary artery disease
- Sleep apnea
- Structural defects of the heart or valves
- Lung disease
- Thyroid gland disorders
- Inflammation of the heart muscle
- Fatigue
- Obesity
HEART RHYTHM CONDITIONS
Sinus tachycardia is a condition where the heart beats faster than normal (over 100 beats per minute), but the rhythm remains regular. It typically occurs during physical exertion, excitement, stress, or as a result of certain disorders such as hyperthyroidism, anemia, or fever. Sinus tachycardia is usually not dangerous and does not require treatment.
The normal heart rate for an adult range from 60 to 100 beats per minute. If the heart rate is consistently lower than this range, the patient likely has bradycardia, while a higher heart rate represents tachycardia. Not all deviations from the normal heart rate are harmful to health, for example, athletes and physically active workers often have a lower heart rate than normal. During sleep, the heart rate can also be lower.
Bradycardia most commonly occurs due to dysfunction of the sinus node or sick sinus syndrome. The sinus node plays an enormous role in the proper functioning of the heart. It sends electrical signals and controls the heart’s rhythm. If everything is functioning correctly, the heart rate will be in the range of 60 to 100 beats per minute, but if it is not working properly, it can send signals slowly.
The most common form of arrhythmia occurs when the electrical signal that causes organized atrial contraction becomes irregular and disorganized. Atrial fibrillation can occur from time to time (paroxysmal AF) or it can be a permanent condition. It can be a factor for stroke, especially for patients who are over 65 years old, diagnosed with high blood pressure, congestive heart failure, diabetes or peripheral vascular disease.
Atrial tachycardia is characterized by a rapid heart rate in the atria due to the occurrence of an ectopic impulse, with a regular rhythm at a frequency of 120-220/min. If the impulse conduction is regular (1:1), the ventricles accelerate, and a true rhythmic supraventricular tachycardia occurs. However, much more common is atrial tachycardia with block, 2:1, 3:1, 4:1 (meaning not every impulse produces a contraction of the ventricles), so the ventricular rate is uneven but usually not accelerated.
Atrial flutter, similar to atrial tachycardia, is characterized by a rapid heart rate. Normally, the atria of the heartbeat evenly at a rate of 60-80 beats per minute. If atrial flutter is present, the atria beat very rapidly but in a regular rhythm of around 90-150 beats per minute, and the ventricles respond unevenly, leading to an irregular and rapid heart rate. Sometimes this condition occurs together with another type of irregular heart rhythm called atrial fibrillation. The main causes of this condition are mitral valve disease, high blood pressure, heart attack, thyroid disease, blood clots in the lungs, stimulants (cocaine, methamphetamines), excessive alcohol consumption, viral infections, and stress caused by other illnesses.
Symptoms
Heart palpitations, dizziness, shortness of breath, fainting, chest pain, anxiety.
Supraventricular Tachycardia includes several other types of rapid heart rhythm that are usually not dangerous, but can cause symptoms of palpitations, fatigue, or shortness of breath. They usually start suddenly and stop suddenly, and can last for minutes or hours, with a fast but steady pulse throughout the episode.
They occur as a result of abnormal transmission of impulses from the atria to the ventricles, resulting in a very fast heart rhythm. The incidence of Supraventricular Tachycardia (SVT) increases with age and is more common in women.
Symptoms
Symptoms vary from person to person. Many people have no symptoms at all. Others have chest pain, rapid heart rate, shortness of breath, fainting, nausea, and loss of consciousness (syncope).
Treatment options include medication or a catheter ablation procedure.
Ventricular Tachycardia occurs as a result of abnormal electrical communication in the chambers of the heart that causes very fast heartbeats. This disorder is very dangerous because the heart beats so fast that sometimes it cannot get enough blood. VT can also develop into ventricular fibrillation (VF), a potentially fatal irregular heart rhythm when the heart stops beating but flutters and stops pumping blood around the body (cardiac arrest).
The most common causes are heart attack, heart failure, illicit drug use, congenital heart defects, previous heart surgery, cardiac trauma, blood chemistry abnormalities (electrolytes), and overactive thyroid gland (hyperthyroidism).
Because VT can lead to ventricular fibrillation, it is considered a serious condition that requires aggressive monitoring and treatment.
If it does not go away on its own, VT usually requires immediate treatment with either medication or an electrical impulse to the heart (electrical cardioversion). Further treatment of VT may include antiarrhythmic drugs or a catheter ablation procedure. Often, people with VT and heart disease are implanted with a device – a defibrillator (ICD) that prevents entry into VF.
The most common cause of cardiac arrest is an arrhythmia called Ventricular Fibrillation – when rapid, erratic electrical impulses cause your ventricles to quiver unnecessarily instead of pumping blood. This leads to a drop in blood pressure and interruption of blood flow to your vital organs resulting in loss of consciousness. Ventricular fibrillation is the most dangerous of all arrhythmias and accounts for half of all cardiac deaths. It can be caused by previous heart damage or an inherited (genetic) heart condition. Sometimes VF can occur during a heart attack (myocardial infarction), because then the heart muscle is more sensitive and susceptible to the occurrence of rhythm disturbances. It is important to understand that Ventricular Fibrillation is an electrical disorder of the heart (not the same as a “heart attack” and may or may not be related to a problem with blocked arteries that supply the heart with blood).
Ventricular Fibrillation is sudden and happens without any warning. It stops the heartbeat. Lack of blood and oxygen throughout the body, especially the brain, is fatal within minutes if not treated promptly.
Although CPR (cardiopulmonary resuscitation) may provide temporary benefit, the only truly effective treatment for VF is defibrillation. Defibrillation is performed by delivering electrical impulses to the heart through paddles placed on the chest that restart the heart back to a normal rhythm.
AV Block – Heart block is a problem with the heart’s electrical system, which powers the heart, regulates heart rhythm, and controls heart rate. This condition is also called atrioventricular (AV) block or cardiac conduction disorder.
Under normal conditions, electrical signals travel from the upper parts of the heart’s atria to the ventricles. The AV node is a cluster of cells that connect electrical activity—like a bridge—from the atria to the ventricles. If you have heart block, the electrical signal does not travel through the AV node to the ventricles. The result is a heart that doesn’t work efficiently, meaning the heart beats slowly or skips a beat and can’t pump blood through its chambers and out to the body like a normal heart does.
AV Block can be of the first, second or third degree, depending on the degree of damage to the electrical signal.
First-degree AV block: The electrical signal impulse reaches the ventricles, but more slowly than it should through the AV node. Impulses are delayed. This is the mildest type of heart block.
Second degree AV block is classified into two categories: Type I and Type II. In second-degree heart block, impulses are occasionally blocked.
- Type I, also called Mobitz Type I or Wenckebach AV Block: This is a less severe form of second-degree heart block. The electrical signal gets slower and slower until the heart skips a beat.
- Type II, also called Mobitz Type II: Although most of the electrical signals occasionally reach the ventricles, some signals do not get through and the heartbeat becomes irregular and slower than normal.
Third degree AV block: The electrical signal from the atria to the ventricles is completely blocked. To compensate, the ventricle usually starts beating on its own, acting as a replacement for the pacemaker, but the heartbeat is slower, often irregular, and unreliable. Third degree blockage seriously affects the heart’s ability to pump blood around your body.
Treatment of AV Block:
If you have first-degree heart block, you probably won’t need treatment.
Second-degree block: If you have second-degree heart block and have symptoms, you may need a pacemaker to keep your heart beating normally. A pacemaker is a small device that sends electrical impulses to your heart.
Third-degree block: Third-degree block is often first discovered during an emergency. Treatment almost always involves a pacemaker.
DIAGNOSIS OF ARRHYTHMIAS
Diagnostic electrophysiological study (EPS) – Performed to identify the location of abnormal electrical pathways in your heart. Electrical wires are inserted into a catheter and run through blood vessels through your groin to your heart, providing information that is critical to diagnosing and treating arrhythmias. While inside the chambers of the heart, the wires record abnormal impulses or heartbeats. Once an abnormality is detected, it can be treated with radiofrequency catheter ablation.
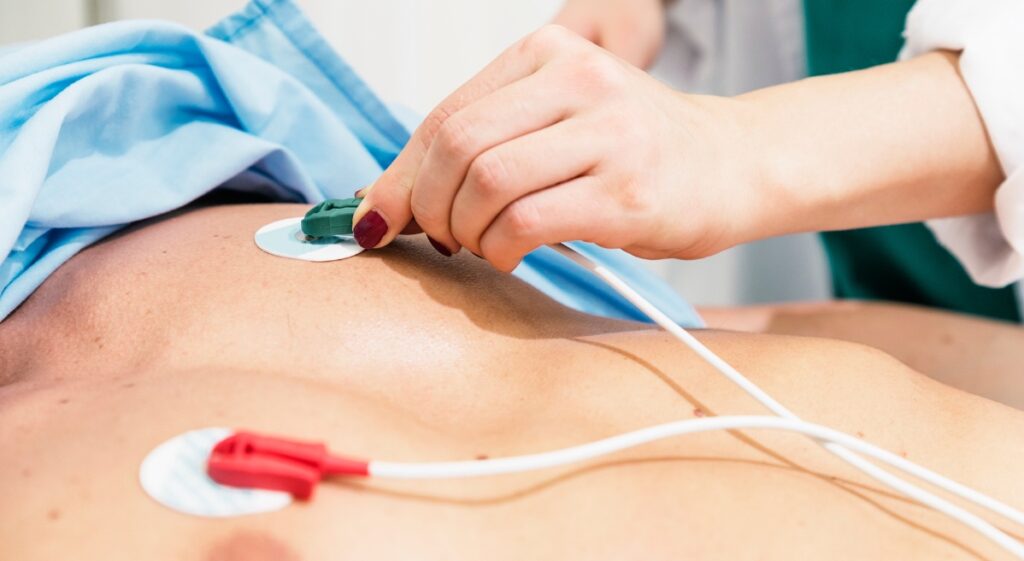
Electrocardiogram (ECG) – is a graphic record of the electrical activity of the heart. ECG – painless and non-invasive test includes data that make it possible to determine the source of arrhythmia symptoms, predict the risk of certain heart conditions, evaluate the effectiveness of drugs that can be used to control heart rhythm disorders, and assess the need for an ablation procedure or the use of an implantable device such as an ICD or pacemaker.
Holter monitor – This is an external device worn by people who may be at high risk of complications from the heart circuit. A Holter monitor automatically records a continuous ECG – the electrical activity of the heart constantly while the person is wearing it. The Holter is usually worn for 24 to 48 hours, after which the doctor removes the device and reads the results.
Loop recorder – An implantable loop recorder (ILR) is a small cardiac recording device that is implanted along the edge of the sternum under the skin. It serves for the differential diagnosis of repeated crises, i.e., loss of consciousness, the cause of which was not detected by a standard multidisciplinary approach. It can be worn for three years, and depending on the detected cause, a further type of treatment is suggested. An implantable loop recorder continuously checks the heartbeat over a long period of time. This means it can see changes in heart rate that other heart rate monitors might miss. For example, it may reveal:
- irregular heartbeats that are short or happen only from time to time
- whether the cause of fainting is a heart problem
- irregular heart rhythms that can lead to a stroke
Here, you can read everything about installing a Loop recorder.
TREATMENT OF ARRHYTHMIAS
Specialized treatments and procedures for patients with arrhythmias
Most arrhythmias are treated with a high cure rate and a low complication rate. At Pulse Cardiology Center, within the Center for Arrhythmias, various therapies are available for the treatment of arrhythmias. Different therapies depend on the condition or cause of the arrhythmia. Some arrhythmias can be treated with medical therapies, while other types of arrhythmias may require special monitoring to aid in diagnosis. Information gathered during monitoring will help determine treatment methods and whether an invasive procedure may be necessary.
Medical therapy – Certain rhythm disorders are treated with antiarrhythmic drugs prescribed by a cardiologist/arrhythmologist/electrophysiologist. Inpatient monitoring during initiation of these drugs is used for rhythm management and antithrombotic therapy.
Devices / Shockers – These devices deliver a controlled electrical impulse to the heart. A defibrillator can actually “shock” the heart back out of a lethal rhythm into a normal heart rhythm. In emergency situations, the devices are external, but most often they are implanted on the patient’s chest under the skin. At the Pulse Cardiology Center, we install pacemakers and ICDs – defibrillators.
Pacemaker – A small electrical device that “paces” the heart when it beats too slowly (bradycardia). A pacemaker is implanted in the chest just under the skin and has insulated leads that are placed inside one of the heart’s chambers. An electrode at the end of the wire touches the heart wall and when an abnormality is detected, the electrode delivers electrical impulses to the heart. The pacemaker can take over from the sinoatrial node, or the heart’s natural pacemaker, when it isn’t working properly. Pacemakers monitor and regulate the heart’s rhythm and transmit electrical impulses to stimulate the heart if it is beating too slowly. Here, you can read everything about pacemaker installation.
Implantable Cardioverter Defibrillators (ICD) – An ICD is a small electrical device that is placed on the chest under the skin. It constantly monitors your heart rate. If it senses a dangerously fast heart rate, it delivers a pulse or shock to the heart and restores a normal rhythm. ICDs are 99% effective in stopping life-threatening arrhythmias and are the most successful therapy for treating ventricular fibrillation, the main cause of SCD. ICDs continuously monitor the heart’s rhythm, functioning as pacemakers for too slow heartbeats and delivering life-saving shocks if a dangerous heart rhythm is detected. Here, you can read everything about installing an ICD defibrillator.
Heart Failure Devices – There are several devices available for patients with low ejection fraction or patients whose heart has a low percentage of pump function that can be augmented by certain pacing patterns. Electrophysiologists are able to implant both the left and right sides of the heart to resynchronize muscle contractions and improve the pumping function of a weakened heart.
RADIOFREQUENCY ABLATIONS WITH 3-D MAPPING
Cardioversion – refers to the process of returning the heart rhythm to normal from an abnormal rhythm. Most planned cardioversions are performed to treat atrial fibrillation, a heart rhythm disorder that occurs in the chambers of the heart. This is an outpatient procedure performed while the patient is awake with necessary sedation. During cardioversion, direct current is used to momentarily depolarize most of the heart’s cells, allowing the sinus node to resume normal pacemaker activity. Practically, the patient is shocked with a defibrillator in order to “restart” the heart’s work and start again with normal heart work. Here, you can read everything about cardioversion.
Ablation – Blocking or scarring abnormal electrical circuits or areas that are causing the problem. This is done by guiding a catheter through the blood vessels to the heart by heating or freezing the problem cells. This causes the nerve cells in a very small area to die, which blocks the area’s circulation and prevents that area from transmitting additional impulses that cause the heart to beat too fast. Candidates for ablation include atrial fibrillation in cases where drug therapy is ineffective or not tolerated.
Pulmonary vein isolation procedure – Atrial bypasses in the left atrium or pulmonary veins are blocked to potentially cure atrial fibrillation. This procedure is suitable for patients who have paroxysmal or persistent AF that does not respond to medical treatments, has complications, or cannot tolerate antiarrhythmics.
AV Node Ablation – This ablation procedure improves symptoms when the cause of atrial fibrillation (Afib) cannot be corrected. The ablation procedure will block the AV node, which is the area in the heart where the atrial and ventricular electrical systems are located, so that the atria can no longer send signals to the ventricles. After AV node ablation, a permanent pacemaker will be implanted to stimulate the ventricles to beat. This will help improve the symptoms of Afib and allow you to stop taking any medications.
Several centers of excellence have been established within the Pulse Cardiology Center. You can get more information about our Centers by clicking on the links: