Narrowing of the coronary arteries occurs due to the buildup of plaque in the arteries that supply the heart muscle. This plaque buildup causes the artery to narrow, a condition known as atherosclerosis, and it disrupts blood flow to the heart. Without proper blood flow, the heart does not receive enough oxygen, which damages the heart muscle and increases the risk of a heart attack.
The difference between a metal stent and a drug-eluting stent
As stents have proven to be an effective solution for coronary artery disease, their quality and functionality have been improved over time. In addition to standard stents, drug-eluting stents (DES) have been used since the 2000s. These stents are developed to reduce the high rate of restenosis and the need for subsequent revascularization with a metal stent.
When a stent is initially placed in an artery, new tissue forms inside and around it from healthy (endothelial) cells that line the artery wall. This tissue prevents blood clotting as it flows through the stent. However, scar tissue can form beneath the healthy tissue and, with its growth, can lead to artery narrowing again. By using a drug-eluting stent, the artery expands, and the drug helps keep the artery open for unobstructed blood flow.
This type of stent provides a permanent solution. Once implanted, it lasts a lifetime, and patients tolerate it well. Clinical trials have shown that the use of drug-eluting stents rarely requires re-intervention.
At PULSE Cardiology Center, modern stents are used that release medication for months to prevent restenosis, providing a long-term solution for narrowing of the coronary arteries.
This does not mean that drug-eluting stents have completely replaced metal stents. Although they do not contain medication, metal stents are not obsolete. Depending on the patient’s health condition, the interventional cardiologist determines the type of stent to be used.
What is the procedure for implanting a drug-eluting stent?
The placement of a drug-eluting stent is performed during a cardiac catheterization procedure. The interventional cardiologist, during this minimally invasive procedure, makes a small incision in the groin or arm and inserts a thin tube – a catheter with a balloon at the end – into the blood vessel.
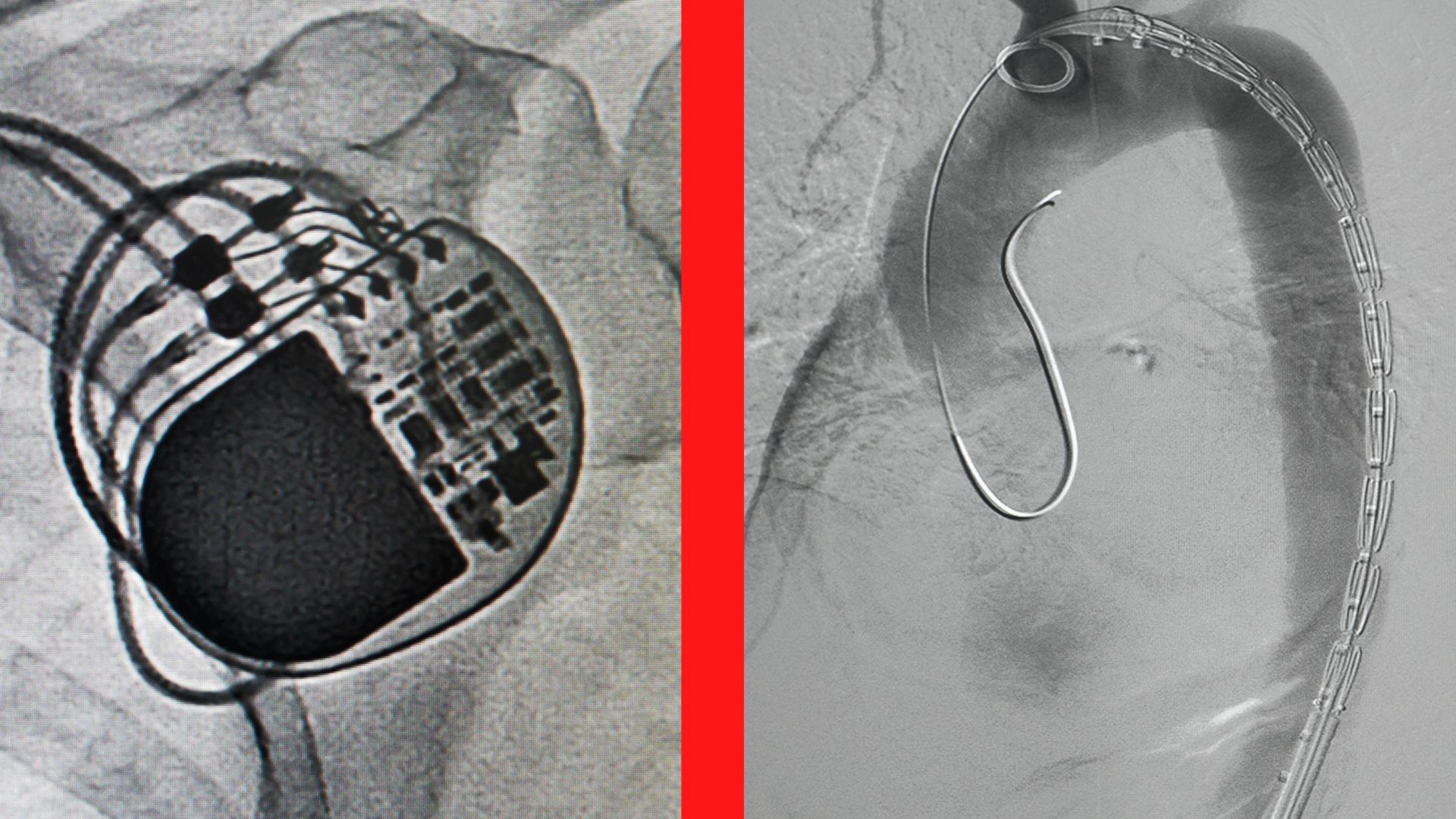
Using contrast dye and X-ray images, the doctor guides the catheter towards the coronary artery. Then, they inflate the balloon and push the plaque against the sides of the artery to open it up. Once the artery is open, the doctor places the drug-eluting stent onto the walls of the artery. After the procedure, the patient must take blood-thinning medications.
Cardiac catheterization is performed in a specialized Angio-suite by experts in interventional cardiology and radiology at the PULSE Cardiology Center.
Advantages of drug-eluting stents
Drug-eluting stents can help reduce plaque buildup in the arteries and increase blood flow to the heart, which can alleviate chest pain.
These types of stents also decrease the chances of artery re-narrowing compared to other treatment methods (such as bare-metal stents or angioplasty). The placement of a stent is also less invasive with a shorter recovery time compared to traditional open-heart surgery (bypass surgery).
Minimal risks of stent implantation
Drug-eluting stents are safe and effective for the majority of people. Like all medications, procedures, and medical devices, there are very small risks involved, including:
- Formation of a blood clot
- Damage to your blood vessel from the catheter
- Infection
- Allergic reaction to the contrast agent
- Allergic reaction to the stent
- Irregular heart rhythm
Anticoagulant drug therapy
Since stent implantation involves the use of anticoagulant medications, it is necessary to consult with your doctor to modify or adjust your current medication therapy.